UASI’s HCC experts Nancy Koors, Vice President of Corporate Development and Mary Stanfill, MBI, RHIA, CCS, CCS-P, FAHIMA, Vice President of Consulting Services recently teamed up with Colleen White, MSM, BSN, RN, CPC, Ambulatory CDI Program Manager at ChristianaCare for a webinar discussing Successful HCC Risk-Adjusted Programs: Tactics to Manage Your Risk-Adjusted Population. Colleen has been with ChristianaCare for 21 years and in the CDI program for 2.5 years.
Below is a transcript of our question and answer session with Colleen during the webinar. ChristianaCare is currently in the ‘optimize’ phase of the Risk Adjustment Maturity Model and Colleen offers powerful perspectives for organizations in all phases. For a breakdown of each phase in the Model, click here.
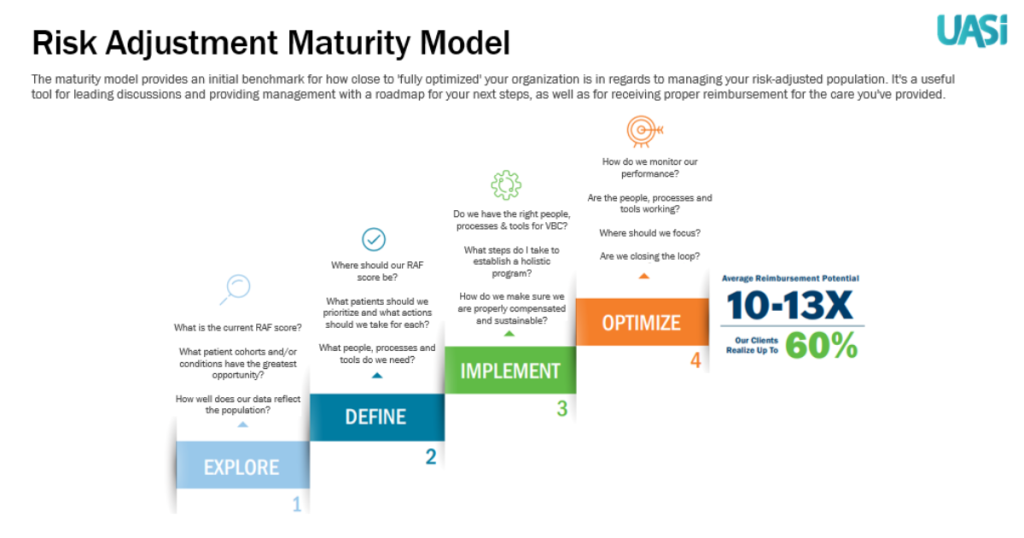
Nancy Koors: What phase are you in and why do you think you are there?
Colleen White: I believe we are in the ‘optimize’ phase. Since it is a fluid model, we constantly must optimize as well as explore, define, and implement. If processes come up that are not working correctly, we go back and reevaluate. We have tied provider incentives to redocumentation of HCCs which goes a long way in provider engagement. We also partner with our payers to make sure that the correlation of data is accurate.
Nancy Koors: How long have you been at it to get to the ‘optimize’ phase?
Colleen White: Our journey began in 2016 with a concept meeting. We identified an opportunity as we started to move towards more value-based contracts. Our pilot included 16 of our primary care practices. In 2017, we added one FTE CDI and concluded that our pilot was successful. From 2017 on, we have continued to grow and add new team members and processes.
Nancy Koors: What was the impetus to have ChristianaCare get started on this journey?
Colleen White: In the payer world, there was a movement to more value-based contracts. Commercial payers usually adopt what CMS is doing a couple years down the road so once CMS started talking about value-based contracts and reimbursement based on the care that the patient receives, rather than fee-for-service, that’s when we started to look at how we can optimize this work now that we are at risk financially.
Nancy Koors: How did you know your organization moved on to the ‘define’ phase?
Colleen White: We realized we needed a more targeted approach after trying a couple different things that worked for a while but not permanently. We also realized we wanted to use our own data instead of receiving it from payers.
Nancy Koors: And how did you attack the ‘implement’ phase?
Colleen White: We started with one person in a pilot and soon added a second person and from there continued to grow the team. We also started prospective reviews, enabled by our EHR platform when they introduced natural language processing. We also continued retrospective chart reviews, but adjusted our process to review charts after the patient visit but before the claim is dropped to ensure visit documentation truly supports the diagnoses. We are now in a hybrid model where we support the providers from a prospective standpoint, as well as a retrospective standpoint, to set them up for success and make sure that they have all the tools necessary to be successful in this work.
Nancy Koors: What are some of your successes and proudest moments in this phase?
Colleen White: I am most proud of our provider education program. I am a very strong proponent of provider education. We need it for our value-based contracts to be successful. We can teach the providers how to document diabetes with hyperglycemia appropriately, but at the end of the day, it is still the provider’s responsibility to do that work. As part of our education program, we developed “One Team, One Message.” We have a tip of the month that we build together as a team and all of the providers get the same message. We truly feel that if we want the providers to be consistent in their documentation and recapture of HCCs, then we need to be consistent in the message that we provide to them. Everything is templated in a standard format and we have also instituted annual education to the providers as part of their learning space. It is a mandatory education for all of our primary care providers to pass with 70% or better.
Nancy Koors: How did this work impact your staff?
Colleen White: We have grown exponentially. We started with one and then a second CDI specialist in 2017. In 2019, the team grew from two to six, so we’ve added four additional CDI team members, and that is when I became part of the CDI world at ChristianaCare. In 2021 we move to a hybrid model where we were setting the provider up for success with prospective reviews.
Nancy Koors: What are your priorities as an organization in the ‘optimize’ phase?
Colleen White: One of our priorities right now is developing a tool for accurate CDI data. We are beginning conversations to create a database tool to accurately capture data reflecting our CDI program’s efforts and answer questions such as: How many queries do we send for the stage of CKD? How many queries do we send to further specify major depressive disorder? Those are things that we’re still tracking on Excel spreadsheets right now.
Nancy Koors: As new specialties and groups of physicians join, do you have a process for onboarding to the program?
Colleen White: We do have a very comprehensive onboarding program for our new primary care practices. We let them know how we are going to support them and we continue to educate them with our education program.
Nancy Koors: There is some curiosity about where this sits in the ChristianaCare organization structure. Where does it sit?
Colleen White: We fall within what ChristianaCare calls our Medical Group. However, in the past three to six months, we have started to partner with our inpatient CDI team, especially when it comes to policy and procedure reviews.
Nancy Koors: If you are in inpatient and you have an outpatient group that is focused on this, why would you need to know or care about this if you are on the inpatient side?
Colleen White: I think it is important to know, just because we are all still CDI specialists involved in clinical documentation integrity. While HCCs don’t necessarily need to be a primary focus of inpatient CDI, it is nice to have an understanding.
Nancy Koors: If there is one thing for our audience to keep in mind as they build their risk adjustment program, what would it be?
Colleen White: Learn how to dance because you’re going to be pivoting, shifting your focus, looking behind to see what you did, where you are, and how you can do it better the next time around. Be flexible and be willing to learn.
If you are interested in finding out where you are in the process of managing your risk-adjusted population, take our 3-Minute Risk Adjustment Checkup. You can also download a white paper covering insights for managing HCCs and risk-adjusted populations on our website.